 Welcome
Welcome
“May all be happy, may all be healed, may all be at peace and may no one ever suffer."
Hot flashes

Hot flashes, also known as hot flashes, are a common symptom experienced by many women during menopause. They are characterized by a sudden feeling of warmth that spreads over the body, often accompanied by sweating, a rapid heartbeat, and a flushed appearance. Hot flashes can be uncomfortable and disruptive, and they can also interfere with a woman's ability to get a good night's sleep.
Hot flashes are caused by changes in the body's hormone levels, particularly a decrease in estrogen. They are also influenced by other factors such as stress, diet, and lifestyle choices.
There are several things that can be done to manage hot flashes. These include:
- Hormone therapy: This involves taking medication that contains estrogen to help alleviate hot flashes and other menopausal symptoms.
- Lifestyle changes: Simple lifestyle changes such as wearing lighter clothing, avoiding spicy foods and alcohol, and practicing stress-reduction techniques like yoga and meditation can help reduce the frequency and severity of hot flashes.
- Medications: Certain antidepressants and blood pressure medications can also help reduce hot flashes.
- Natural remedies: Some natural remedies such as black cohosh, soy, and flaxseed may also provide relief from hot flashes. However, it's important to talk to your doctor before trying any natural remedies, as they may interact with other medications you are taking or have side effects.
If you are experiencing hot flashes, it's important to talk to your doctor to discuss the best treatment options for you.
Research Papers
Disease Signs and Symptoms
- Red skin
- Rapid heartbeat (tachycardia)
- Perspiration, mostly on upper body
- Anxiety
- A flushed appearance with red, blotchy skin
- A chilled feeling as the hot flash lets up
Disease Causes
Hot flashes
Hot flashes are most commonly caused by changing hormone levels before, during and after menopause. It's not clear exactly how hormonal changes cause hot flashes. But most research suggests that hot flashes occur when decreased estrogen levels cause your body's thermostat (hypothalamus) to become more sensitive to slight changes in body temperature. When the hypothalamus thinks your body is too warm, it starts a chain of events — a hot flash — to cool you down.
Rarely, hot flashes and nights sweats are caused by something other than menopause. Other potential causes include medication side effects, problems with your thyroid, certain cancers and side effects of cancer treatment.
Disease Prevents
Disease Treatments
The most effective way to relieve the discomfort of hot flashes is to take estrogen, but taking this hormone carries risks. If estrogen is appropriate for you and you start it within 10 years of your last menstrual period or before age 60, the benefits can be greater than the risks.
Medications such as antidepressants and anti-seizure drugs also might help reduce hot flashes, although they're less effective than hormones.
Discuss the pros and cons of various treatments with your doctor. If hot flashes don't interfere with your life, you probably don't need treatment. Hot flashes subside gradually for most women, even without treatment, but it can take several years for them to stop.
Hormone therapy
Estrogen is the primary hormone used to reduce hot flashes. Most women who have had a hysterectomy can take estrogen alone. But if you still have a uterus, you should take progesterone with estrogen to protect against cancer of the lining of the uterus (endometrial cancer).
With either regimen, the therapy needs to be tailored to your needs. Guidelines suggest using the smallest effective dose for symptom control. How long you use the treatment depends on the balance of your risks and benefits from hormone therapy. The goal is to optimize your quality of life.
Some women who take progesterone with estrogen therapy experience progesterone-related side effects. For women who can't tolerate oral progesterone, a combination drug of bazedoxifene with conjugated estrogens (Duavee) is also approved for treating menopausal symptoms. Like progesterone, taking bazedoxifene with estrogen may help you avoid the increased risk of endometrial cancer from estrogen alone. Bazedoxifene might also protect your bones.
If you have had or are at risk of breast or endometrial cancer, heart disease, stroke or blood clots, talk to your doctor about whether estrogen therapy is right for you.
Antidepressants
A low-dose form of paroxetine (Brisdelle) is the only nonhormone treatment for hot flashes approved by the U.S. Food and Drug Administration. Other antidepressants that have been used to treat hot flashes include:
- Venlafaxine (Effexor XR)
- Paroxetine (Paxil, Pexeva)
- Citalopram (Celexa)
- Escitalopram (Lexapro)
These medications aren't as effective as hormone therapy for severe hot flashes, but they can be helpful to women who can't use hormones. Possible side effects include nausea, difficulty sleeping or drowsiness, weight gain, dry mouth or sexual dysfunction.
Other prescription medications
Other medications that might offer relief for some women include:
- Gabapentin (Neurontin, Gralise, others). Gabapentin is an anti-seizure medication that's moderately effective in reducing hot flashes. Side effects can include drowsiness, dizziness, water retention in the limbs (edema) and fatigue.
- Pregabalin (Lyrica). Pregabalin is another anti-seizure medication that can be effective in reducing hot flashes. Side effects can include dizziness, drowsiness, difficulty concentrating and weight gain.
- Oxybutynin (Ditropan XL, Oxytrol). Oxybutynin is a pill or patch most often used to treat urinary conditions like overactive bladder. It may also help relieve hot flashes in some women. Side effects can include dry mouth, dry eyes, constipation, nausea and dizziness.
- Clonidine (Catapres, Kapvay, others). Clonidine, a pill or patch typically used to treat high blood pressure, might provide some relief from hot flashes. Side effects include dizziness, drowsiness, dry mouth and constipation.
Nerve block procedure
A procedure known as stellate ganglian block has shown promise for treating moderate to severe hot flashes, but more research is needed. It involves injecting an anesthetic into a nerve cluster in the neck. The treatment has been used for pain management. Side effects include pain and bruising at the injection site.
Disease Diagnoses
Disease Allopathic Generics
Disease Ayurvedic Generics
Disease Homeopathic Generics
Disease yoga
Hot flashes and Learn More about Diseases
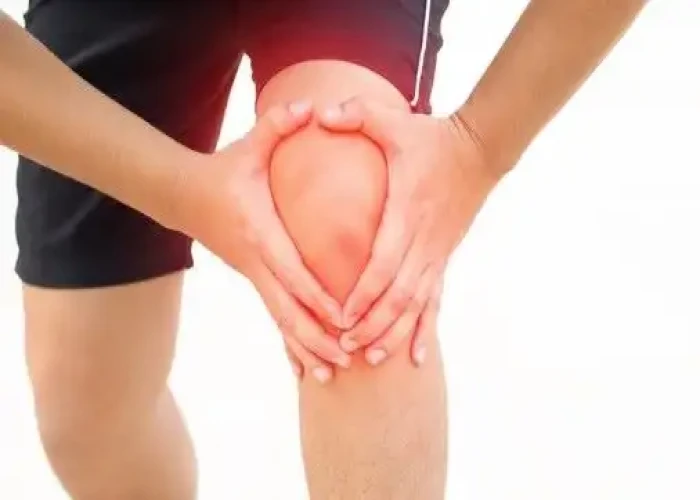
Swollen knee
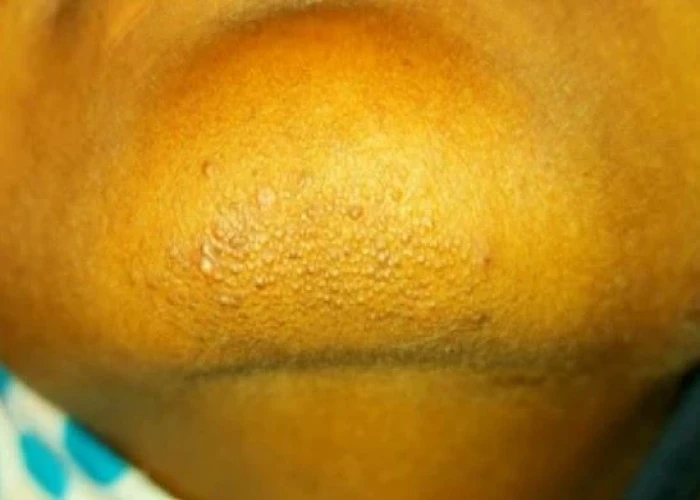
Lichen nitidus
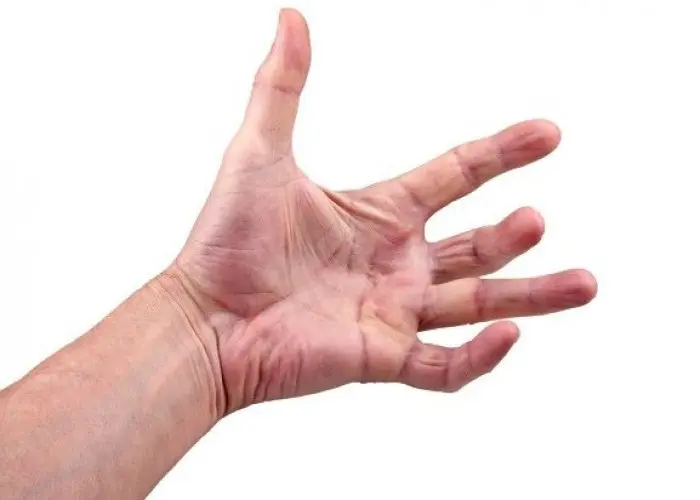
Dupuytren's contracture
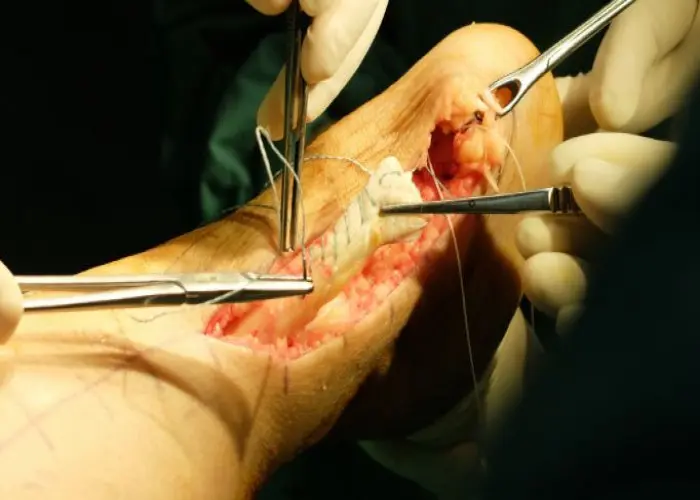
Achilles tendinitis
Urine color

Worms
Placenta previa

Hepatitis B
hot flashes, গরম ঝলকানি
To be happy, beautiful, healthy, wealthy, hale and long-lived stay with DM3S.
