Welcome
Welcome
“May all be happy, may all be healed, may all be at peace and may no one ever suffer."
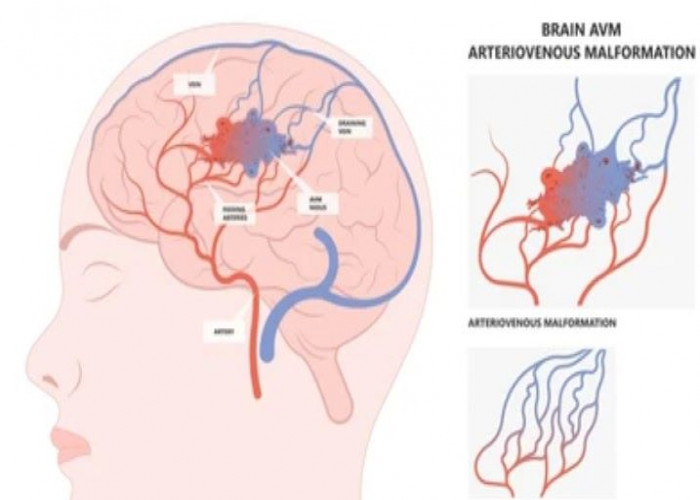
Cavernous malformations

Cavernous malformations, also known as cerebral cavernous malformations or cavernomas, are a type of vascular abnormality in the brain that involves small, thin-walled blood vessels with enlarged and irregular spaces. These malformations can occur sporadically or may be inherited in an autosomal dominant pattern, and may cause a range of symptoms depending on their location and size, such as headache, seizure, weakness, numbness, or difficulty speaking. In some cases, cavernous malformations may not cause any symptoms and may be discovered incidentally on imaging studies done for other reasons. Treatment options for cavernous malformations depend on the location and size of the malformation, as well as the individual's age, health status, and symptoms. In some cases, observation and monitoring may be recommended, while in other cases, surgical removal or radiation therapy may be necessary to reduce the risk of bleeding or other complications. It is important for individuals with cavernous malformations to work closely with a healthcare provider to develop a personalized treatment plan and monitor their condition over time.
Research Papers
Disease Signs and Symptoms
- Headaches
- Nausea or vomiting
- Speech problems
- Weakness
- Numbness
- Difficulty speaking
- Blurred vision of eye
- Double vision (diplopia)
- Lose balance
Disease Causes
Cavernous malformations
Most CCMs occur as a single formation, without an apparent cause and without any family history.
However, roughly 20 percent of affected people have a familial (inherited) form of the disorder. In many cases, such people can identify similarly affected family members, most often with multiple malformations. A diagnosis of the inherited form can be confirmed by genetic testing.
Some CCMs can also occur following focal brain radiation therapy.
Disease Prevents
Disease Treatments
Doctors trained in brain and nervous system conditions (neurologists and cerebrovascular neurologists), brain and nervous system surgery (neurosurgeons), brain imaging (neuroradiologists), and other specialties work with you to treat CCMs as well as other neurological conditions.
Your treatment may include:
- Observation. If you're not experiencing symptoms, your doctor may initially decide to monitor your cavernous malformation, especially since risk is generally lower for those who are non-symptomatic. Sometimes intermittent testing such as magnetic resonance imaging (MRI) is recommended to watch for any changes in the malformation. Let your doctor know right away about any changes in your symptoms.
- Medications. If you have seizures related to a cavernous malformation, you may be prescribed medications to stop the seizures.
- Surgery. If you're experiencing symptoms related to a cavernous malformation that can be reached surgically, your doctor may recommend surgery to remove the malformation.
Potential future treatments
Several imaging technology areas hold promise for both improving predictions of the course of disease in some specific contexts and for enhancing the level of information available about a particular individual's disease state, including potential advances in imaging through quantitative susceptibility mapping (QSM), permeability imaging using dynamic contrast-enhanced MRI, and the use of alternative MRI contrast agents such as ferumoxytol. While still under investigation, such developments hold promise for enhanced imaging that may lead to more precise and effective clinical care in the future.
Disease Diagnoses
Disease Allopathic Generics
Disease Ayurvedic Generics
Disease Homeopathic Generics
Disease yoga
Cavernous malformations and Learn More about Diseases

Neck pain

Syphilis
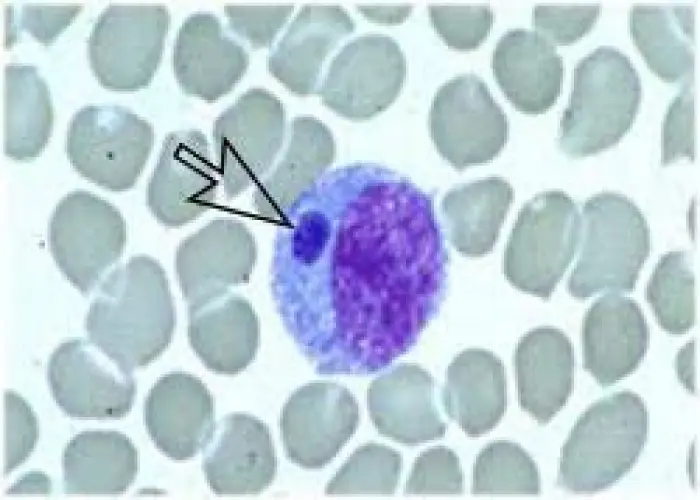
Ehrlichiosis and anaplasmosis

Cavernous malformations
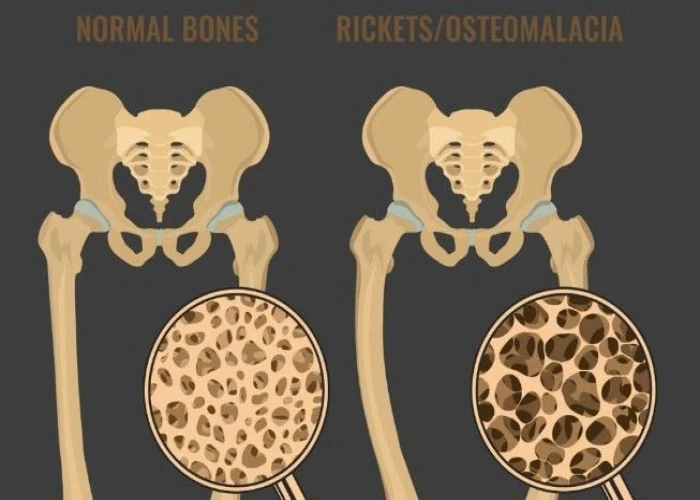
Osteomalacia
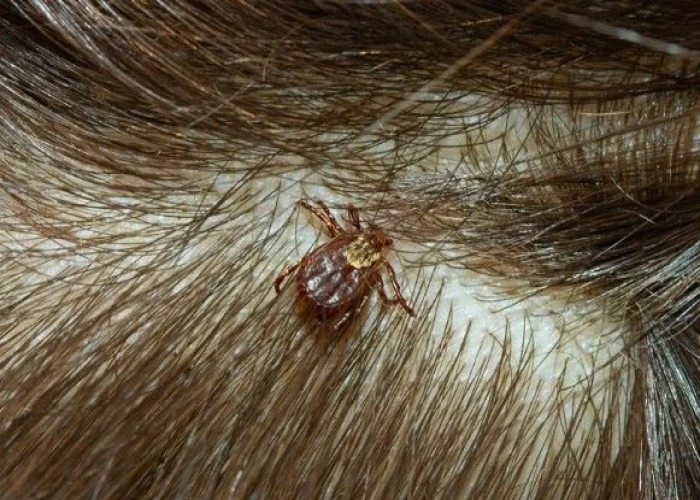
Rocky Mountain spotted fever
Hamstring injury

Nicotine dependence
Cavernous malformations, Cavernous hemangioma, Cavernoma, ক্যাভনরাস বিকৃতি
To be happy, beautiful, healthy, wealthy, hale and long-lived stay with DM3S.